Healthcare delivery has shifted beyond hospital walls, with providers increasingly using digital platforms to consult, monitor, and engage with patients remotely. This shift has made terms like telehealth and telemedicine more common, yet they are often used interchangeably despite having distinct roles in care delivery.
Understanding the difference between telehealth and telemedicine is essential when planning patient care strategies or building digital health solutions. While both enable remote care, they differ in scope, use cases, and long-term value. This guide breaks down telehealth vs telemedicine, helping you identify the right approach based on how care is delivered and experienced.
Understanding Telehealth as a Complete Care Ecosystem
Telehealth refers to the use of digital technologies to deliver a broad range of healthcare services, including clinical care, patient education, remote monitoring, and administrative support. It helps providers to take care of patient health even when they are not physically in the same place, assisting in real-time and continuity care.
Instead of relying solely on consultations, telehealth is a system-level model that integrates various aspects of healthcare into a single continuous process. It facilitates the care delivery process, monitoring, and periodic improvement, particularly among patients requiring frequent checkups or continuous involvement.
In essence, telehealth services involve remote patient monitoring where patient information is monitored in real-time, along with preventive care and chronic disease management programs. Patient engagement apps and mobile health apps assist patients in remaining active in their care, and care coordination systems facilitate provider-administrator communication.
The wider strategy makes telehealth a significant element of remote healthcare service, particularly when the aim is to develop scalable and interconnected digital healthcare systems that go beyond one-time treatment.
Understanding Telemedicine as a Clinical Service Model
Telemedicine is a subset of telehealth that focuses on delivering clinical services such as diagnosis, consultation, and treatment through digital communication technologies. It allows healthcare providers to communicate with patients digitally, providing treatment and consultations without having to visit them physically.
The focus here is direct patient-doctor interaction. The telemedicine services are meant to recreate the process of a clinical encounter in a virtual environment and therefore work best in cases where urgent medical care is needed, but the physical presence is not necessary.
The primary features of telemedicine app are video sessions (where patients are able to communicate directly with doctors in real-time) as well as diagnosis and treatment, depending on any reported symptoms or shared medical data. Telemedicine solutions also include e-prescriptions and follow-ups, which guarantee continuity of care when the initial consultation is over.
It makes telemedicine particularly useful in the context of immediate and episodic care provision, when patients require immediate access to medical expertise by visiting a physician via the internet without following the conventional clinical processes.
Telehealth vs Telemedicine: A Structural Comparison
Understanding the structural differences helps understand where each of the models can be applied in the real world when it comes to healthcare delivery. Although they both use digital technologies, their potential, functionality, and effect on patient care are quite different.
| Aspect | Telehealth | Telemedicine |
|---|---|---|
| Scope and Coverage | Broad ecosystem that includes clinical and non-clinical services | Focused only on clinical services |
| Type of Care Delivery | Continuous, preventive, and long-term care | Episodic, issue-based care |
| Technologies Involved | RPM devices, mobile health apps, patient portals, analytics platforms | Video conferencing tools, clinical communication platforms |
| Stakeholders Involved | Patients, doctors, caregivers, health coaches, admin staff | Primarily patients and healthcare providers |
| Level of Patient Engagement | High, with ongoing interaction and health tracking | Limited to consultation-based interaction |
| Integration with Healthcare Systems | Deep integration with EHRs, monitoring systems, and care workflows | Moderate integration focused on clinical data exchange |
This telehealth versus telemedicine comparison demonstrates that telehealth is oriented to more connected and long-term care, whereas telemedicine is set up to achieve specific clinical communication.
Telemedicine vs Telehealth Examples in Real-World Healthcare
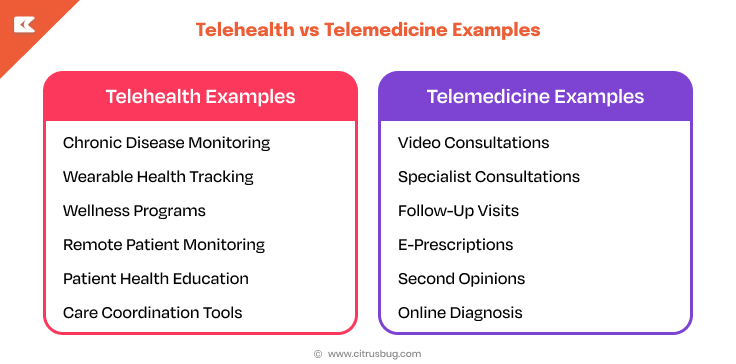
It is easier to see how these models are implemented by looking at practical scenarios. These telehealth vs telemedicine examples highlight how each approach supports different types of care delivery.
Preventive and Continuous Care (Telehealth-Led)
Telehealth is extensively applicable in those cases when care must be proactive and continuing. Remote patient monitoring enables healthcare professionals to manage a condition such as diabetes or heart disease with the help of connected devices, which transmit real-time information.
Wearable devices and mobile applications assist patients in tracking their daily health parameters such as activity levels, heart rate or glucose levels. In addition to this, virtual wellness apps and patient education platforms keep the users engaged and informed, and in this way assist in long-term health management.
Clinical and On-Demand Care (Telemedicine-Led)
Telemedicine is more suited for situations that require direct medical attention. Patients are able to book video appointments on common diseases, to discuss their symptoms and get treatment advice without the need to attend a clinic.
It is also applied in specialist consultations and second opinions, particularly where there is a lack of access to experts. Another typical use case of telemedicine is the follow-up visit after the treatment, which serves as a method of maintaining continuity without direct visits.
Integrated Care Models (Combined Approach)
Most healthcare providers today are integrating both models to provide more comprehensive care. For example, post-surgery recovery programs often include virtual consultations along with remote monitoring to track patient progress.
Chronic care management platforms also integrate telehealth and telemedicine, allowing patients to consult doctors when needed while continuously sharing health data through connected systems.
How Each Model Impacts Patient Care and Outcomes
The difference between telehealth and telemedicine becomes more practical when you look at how each model affects care delivery, patient experience, and clinical outcomes.
Continuity of Care
Telehealth is meant to provide continued care. It promotes ongoing observation, frequent check-ups, and chronic care. This makes it highly effective for preventive care and chronic disease management, where consistent engagement improves outcomes over time.
Telemedicine is more oriented toward individual interactions. It is applied in cases when a patient requires immediate medical consultation, diagnosis, or treatment of a certain problem without constant monitoring.
Access to Care
Telemedicine enhances accessibility by allowing patients to reach doctors in real time, no matter where they are. It minimizes the wait duration and assists in the resolution of urgent health issues by using virtual doctor consultations.
Telehealth increases access differently. It secures the continuity of care to the patient even without a consultation, through remote healthcare services, such as monitoring devices and digital platforms.
Patient Experience
Telehealth provides a more engaged patient experience. Patients engage actively in monitoring their well-being, adhering to treatment plans, and remaining active with the help of digital devices.
Telemedicine is convenient and fast. Patients are able to solve problems with their health within a short time without having to visit a clinic, which is suitable for episodic care requirements.
Provider Efficiency and Workflows
Telehealth encourages well-organized and data-intensive processes by providing practitioners with access to patient information at all times. This assists in planning the early intervention and care.
Telemedicine makes clinical practices easier because it minimizes patient visits and manages them online. It enables the providers to handle a larger number of patients in less time.
This comparison draws out the unique advantages of telehealth and telemedicine and how each model has a different impact on enhancing patient care and healthcare delivery.
Technologies Enabling Telehealth and Telemedicine
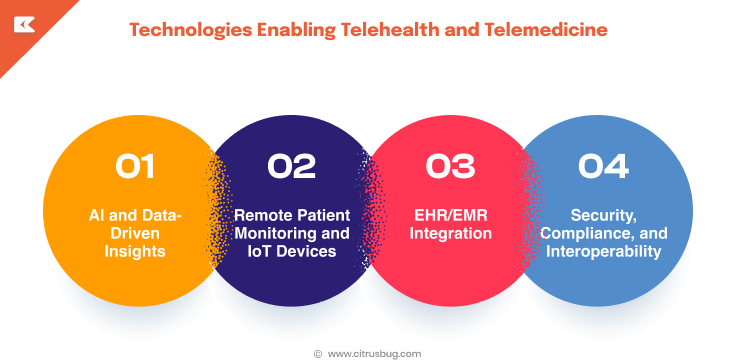
The modern virtual care relies on a complex of innovative technologies that allow providing real-time communication, constant monitoring, and safe data exchange. Such technologies are the core of the scalable and dependable delivery of healthcare digitally.
→ AI and Data-Driven Insights
AI in telehealth is important in processing extensive amounts of patient data, assessing trends, and aiding clinical decision-making. It also assists in automating the routine, like patient triaging, alerts, and follow-ups, enhancing the efficiency of the overall care.
→ Remote Patient Monitoring and IoT Devices
RPM systems rely on interconnected devices that measure real-time health measurements, such as vital signs, activity, and condition-specific measurements. Through these insights, providers are able to monitor the health of the patients in real-time and intervene early in case of risks being identified.
→ EHR/EMR Integration
Electronic health records integration will ensure that the patient information is always updated and accessible across systems. This level of healthcare interoperability enhances improved coordination among providers and minimizes gaps in care delivery.
→ Security, Compliance, and Interoperability
Telemedicine and telehealth systems should adhere to high data security and compliance principles. Encryption, role-based access, and secure data exchange protocols assist in securing sensitive information and removing the block of system communications.
Cost and Implementation Considerations
The investment required depends on the scope, integrations, and long-term goals of the platform. This telehealth vs telemedicine cost analysis indicates the most important differences in the development timeline, complexity and the overall cost.
| Factor | Telehealth Platforms | Telemedicine Software |
|---|---|---|
| Development Scope | Broad scope including monitoring, engagement, analytics, and care coordination features | Focused scope centered on consultations and basic clinical workflows |
| Development Time | Typically 6–12+ months depending on integrations and feature depth | Typically 2–4 months for a functional MVP |
| Estimated Cost | $80,000 to $250,000+ based on complexity and integrations | $25,000 to $80,000 depending on features and scale |
| Complexity | High, due to multiple modules and interconnected systems | Moderate, with a limited and well-defined feature set |
| Infrastructure Needs | Requires integration with EHRs, IoT devices, and other healthcare technology platforms | Primarily depends on video communication and basic data exchange systems |
| Compliance Requirements | More extensive due to continuous data collection and multiple touchpoints | Standard compliance focused on secure consultations and patient data |
| Time to Market | Longer due to broader functionality and system dependencies | Faster deployment with fewer dependencies |
| Scalability | Designed for long-term expansion and continuous care models | Scalable but may require feature expansion over time |
How to Choose the Right Approach for Your Healthcare Needs
Choosing between telehealth and telemedicine depends on how care is delivered, who the patients are, and how the solution is expected to scale over time.
→ Care Delivery Model
Telehealth is more appropriate in the context of long-term care, such as preventive measures and continuous treatment. Telemedicine is effective in episodic care, when the patient requires urgent consultations or treatment on a particular health issue.
→ Patient Demographics
Telehealth helps patients who need constant care, including those with chronic disorders or recovery needs. Telemedicine suits general users having occasional consultations or follow-ups.
→ Business and Product Goals
Telehealth is the right choice when building a comprehensive digital healthcare ecosystem with multiple services. Telemedicine is more suitable for limited solutions with a focus on virtual consultations and clinical interactions.
→ Budget and Time-to-Market
Telemedicine can be launched faster and with less start-up capital, so it is appropriate when minimum viable products (MVP) are needed. Telehealth is more expensive to invest in initially, but it is more scalable in the long run.
Future Trends in Virtual Healthcare
Virtual healthcare delivery is evolving beyond basic consultations, driven by advancements in technology and changing patient expectations. These healthcare trends are defining the design, delivery, and scale of digital healthcare solutions.
-
Growth of Integrated Care Platforms
Healthcare practitioners are shifting to convergent systems that bring consultations, remote monitoring, and engagement with patients within one system. This change promotes more integrated and continuous care experiences.
-
Expansion of AI-Driven Diagnostics
AI is now a clinical cornerstone, with the diagnostic market hitting $3.79 billion in 2026 at a 42% growth rate. These digital healthcare solutions enable high-speed processing of complex medical imaging for earlier intervention.
-
Increasing Adoption of Wearable Devices
Wearables are now essential medical tools, with the global market reaching $117 billion this year. Recent data shows 35% of U.S. adults use wearable devices, while 40% utilize healthcare-related applications.
-
Shift Toward Personalized and Data-Driven Healthcare
Virtual care is increasingly becoming personalized, with treatment plans and advice being made based on patient data and behavior. This method assists in enhancing results and involvement with patients in the long run.
Conclusion
Telehealth and telemedicine both play important roles in modern healthcare, but they serve different purposes. Telehealth supports continuous, connected care through monitoring and patient engagement, while telemedicine focuses on delivering quick, clinical consultations when immediate attention is needed.
Choosing between the two depends on how care is delivered, the needs of your patients, and how you plan to scale your solution over time. In many cases, combining both approaches creates a more flexible and effective care model.
If you are planning to build a healthcare solution, choosing the right technology and architecture is critical. At Citrusbug Technolabs, we help healthcare organizations with custom telemedicine app development and scalable telehealth platform development, enabling them to deliver secure, efficient, and future-ready digital care experiences.
FAQs
What is the difference between telehealth and telemedicine?
Telehealth covers broader healthcare services, including monitoring and education, while telemedicine focuses on virtual clinical consultations and treatment.
Which is better for continuous patient care?
Telehealth is ideal for ongoing care, chronic condition monitoring, and preventive programs, providing consistent engagement and long-term support.
Can telemedicine handle specialist consultations?
Yes, telemedicine enables specialist advice, second opinions, and follow-ups through secure virtual consultations, reducing the need for in-person visits.
How do I choose between telehealth and telemedicine?
Decide based on care model, patient needs, budget, and scalability. Telehealth suits continuous care; telemedicine fits immediate or episodic consultations.